
Insights & Analysis
There’s one constant in healthcare: change. Count on us to break down the trends so you can stay up to date. Follow our take on each piece of this deep, intertwined, and often perplexing industry to find opportunities and practical approaches to move healthcare forward.
MolDX May Be the Norm, but Is It the Future?
With over 16,000 genetic tests already on the market and thousands more in development, stakeholders cannot ignore the rapidly evolving field of personalized medicine.
Avalere Observations on a Potential Approach to Essential Health Benefits
The Affordable Care Act (ACA) requires health plans in the individual and small group markets-both inside and outside exchanges-to offer essential health benefits (EHB).

CY 2015 OPPS/ASC Proposed Rule Makes Refinements to Last Year’s Significant Changes to the Outpatient Payment System
On July 3, CMS released the Calendar Year (CY) 2015 Outpatient Prospective Payment System (OPPS) and Ambulatory Surgical Center (ASC) proposed rule.

CY 2015 MPFS Proposed Rule Details Chronic Care Management Payment, Increases Transparency of Code Revaluations, Continues Implementation of Quality Programs
On July 3, CMS released the Calendar Year (CY) 2015 Medicare Physician Fee Schedule (MPFS) proposed rule.

CMS Proposes Flat Payment and New Quality Measures for Dialysis Facilities
In the Calendar Year (CY) 2015 End Stage Renal Disease (ESRD) Prospective Payment System (PPS) proposed rule released on July 2, CMS proposes a 2015 base per treatment rate of $239.33, up slightly from $239.02 in CY 2014.

CVS Caremark Announces New Partnerships with Medicare ACOs to Reduce Drug Spending
On June 27, CVS Caremark announced partnerships with seven additional Medicare accountable care organizations (ACOs) to improve pharmacy care and reduce drug spending for beneficiaries enrolled in CVS' SilverScript Medicare Prescription Drug Plan (PDP).

NCQA Releases New Technical Specifications for the 2015 Edition of HEDIS
NCQA has released new technical specifications for the 2015 version of Health Effectiveness Data and Information Set (HEDIS) to include four new measures, changes to seven measures, the retirement of two measures and minimal changes to various other measures.

Supreme Court Hobby Lobby Decision Limits Contraception Coverage Mandate
In a 5-4 ruling on June 30, the U.S. Supreme Court issued a majority opinion on Burwell v. Hobby Lobby Stores, Inc., holding that the contraceptive mandate violates the Religious Freedom Restoration Act (RFRA) as applied to closely held, for-profit corporations.

Addressing Sustainability and Informatics Challenges for Clinical Data Registries
In the spring 2014 edition of the Journal of Health Information Management (JHiM), Avalere's Chris Boone published an article addressing modern-day challenges to clinical data registries (CDR).
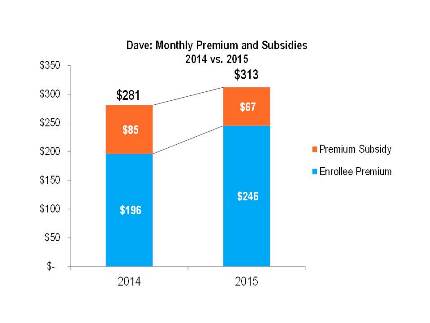
Exchange Plan Renewals: Many Consumers Face Sizeable Premium Increases in 2015 Unless They Switch Plans
New analysis from Avalere Health finds that many consumers in exchange plans who receive federal assistance to reduce their monthly premiums will face substantial premium increases unless they switch insurance plans in 2015.

Differences in FDA Communication Practices Result in Increased Review Times for Devices
As the medical device industry prepares for the next round of user fee negotiations, manufacturer representatives must consider the importance of FDA's approval process transparency, and regular interactive communication.

Avalere Analysis: 90% of Companies Offer Cost-Sharing Assistance to Exchange Enrollees, But Program Characteristics Vary Widely
A recently-completed Avalere Health survey finds that while 90 percent of pharmaceutical and biotech manufacturers are offering cost-sharing assistance to exchange patients, the type of support, generosity and program structure vary widely.

MedPAC Advises CMS to Make Critical Changes to its Medicare ACO Programs
On June 16, MedPAC issued a letter to CMS, advising the agency to make critical changes to its two accountable care organization (ACO) programs-the Pioneer demonstration and Medicare Shared Savings Program (MSSP).

An Opportunity for SNFs Through New Payment Models
In this week's edition of McKnight's Long-Term Care, Jeff Terkowitz wrote a guest column discussing new payment models, and the opportunities they present for SNFs.
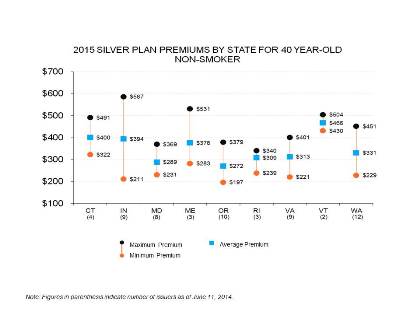
Avalere Analysis: Average Exchange Premiums Rise Modestly in 2015 and Variation Increases
New analysis from Avalere Health finds that average proposed premiums for individual market exchange plans will increase modestly in 2015, based on initial rate filings in nine states.

Diagnostic Laboratory Industry Negotiates FDA’s Revised Standards
As the laboratory testing community continues to weather recent policy changes in both regulatory and reimbursement areas - there has been yet another development.

Washington State Rate Analysis: Carriers with Low 2014 Market Share Hold Down Premiums in 2015
A new analysis from Avalere Health finds that proposed rate increases for 2015 exchange plans in Washington state were lowest among carriers with the smallest share of the 2014 market.

New WellPoint Program Will Pay Physicians For Adhering To Oncology Pathways
On May 28 WellPoint/Anthem BlueCross BlueShield announced the launch of the WellPoint Cancer Care Quality Program - a new pay-for-adherence initiative which incentivizes physicians to follow certain evidence-based WellPoint Cancer Treatment Pathways.

Avalere Analysis: Cost-Sharing for Specialty Medicines
In a June 2014 analysis, Avalere analyzed 123 silver exchange plan formularies to evaluate tier placement.

CMS Delays Implementation of AMP-Based FULs, Originally Scheduled for July
On June 2, CMS announced that it will not finalize the Average Manufacture Price (AMP) based Federal Upper Limits (FULs) for reimbursement of multiple source drugs in Medicaid in July 2014, as expected.


